VETERINARY RESOURCES
Urinary incontinence in the dog
Julie K. Byron DVM, MS, DACVIM
The Ohio State University
College of Veterinary Medicine

Introduction
Urinary incontinence is a common problem encountered in small animal practice. There are a number of causes including congenital anatomic abnormalities, urine retention and overflow incontinence, and sphincter incompetence. The timing of onset of incontinence and the ability of the dog to empty its bladder as well as changes in behavior are important in determining the underlying cause. This review will focus on two of the most common causes of urinary incontinence including urethral sphincter mechanism incompetence (USMI), and functional urethral obstruction or detrusor urethral dyssynergia (DUD).
History and Diagnosis
A careful history is essential when discussing incontinence with pet owners. It must be distinguished from behavioral problems, polyuria, or pollakiuria, and it is important to establish that the animal is unconscious of the passage of urine. Young dogs that have never been continent or have been ‘difficult to housetrain’ should be evaluated for congenital abnormalities such as ectopic ureters. Patients whose incontinence has developed along with an increase in water intake should be evaluated for disorders causing polyuria and polydipsia. The physical examination should include a rectal examination with careful palpation of the urethra. Obstructive processes such as urethral neoplasia and prostatic hyperplasia can often be diagnosed this way. If possible, the dog should be observed while urinating. This is particularly important in males, since functional obstruction and overflow incontinence may be more common than we have previously thought. Dogs that have a narrow urine stream, exhibit strainguria, or only drip urine should have a residual urine volume measured after voiding. Finally, the dog should have a neurologic and orthopedic evaluation if it is unable to posture normally to urinate. This can lead to incomplete emptying of the bladder and incontinence.
All patients with urinary incontinence should receive a urinalysis with sediment examination. While the leakage of urine may be exacerbated by a urinary tract infection, the incontinence itself may predispose the patient to a UTI. It should be kept in mind that there is debate as to whether treating dogs with bacteriuria that lack signs such as stranguria, or dysuria is appropriate. Bloodwork is indicated if the patient has a low urine specific gravity, particularly in the face of dehydration. Most dogs with incontinence develop it as young or middle-aged animals and older onset patients may require additional diagnostic investigation as to an underlying cause. Some dogs may have mild USMI, but are rarely incontinent, until a secondary factor such as increased urine volume comes into play. If the underlying reason for polyuria can be addressed, the incontinence may improve.
Urethral Sphincter Mechanism Incompetence
Urethral sphincter mechanism incompetence (USMI) is the most common cause of urinary incontinence in dogs affecting up to 20% of neutered female dogs and 30% of those over 20 kg. It is less commonly reported in intact and neutered dogs of both sexes. The underlying mechanism is likely multifactorial involving the pituitary-gonadal axis, the anatomic structure of the lower urinary tract, and the integrity and tissue characteristics of its supporting structures. In most dogs it occurs within 3 years of neutering, although in many it may not become a major problem until later in life when it can be complicated by diseases that cause polyuria and polydipsia. Among the most common breeds affected are the Old English sheepdog, Doberman pinscher, Boxer, German Shepherd Dog, and Weimeraner. A recent study indicates that earlier neutering may increase the risk of development of USMI in dogs with a projected adult body weight greater than 15 kg.
Pathophysiology
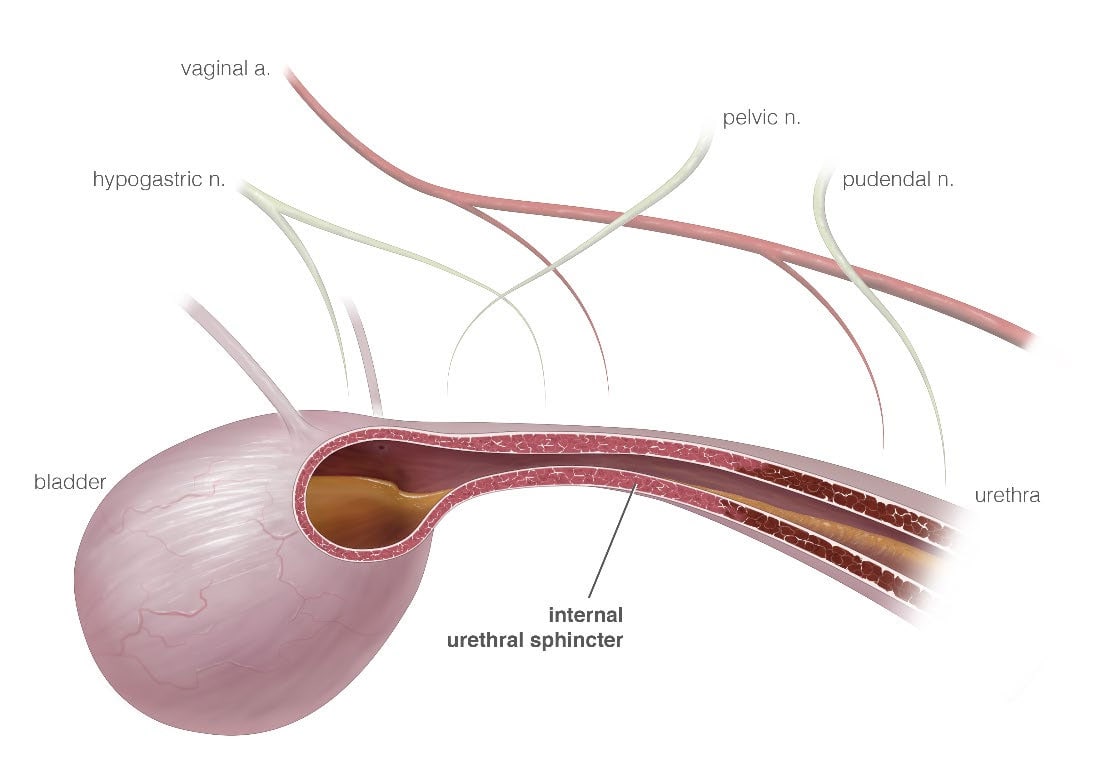
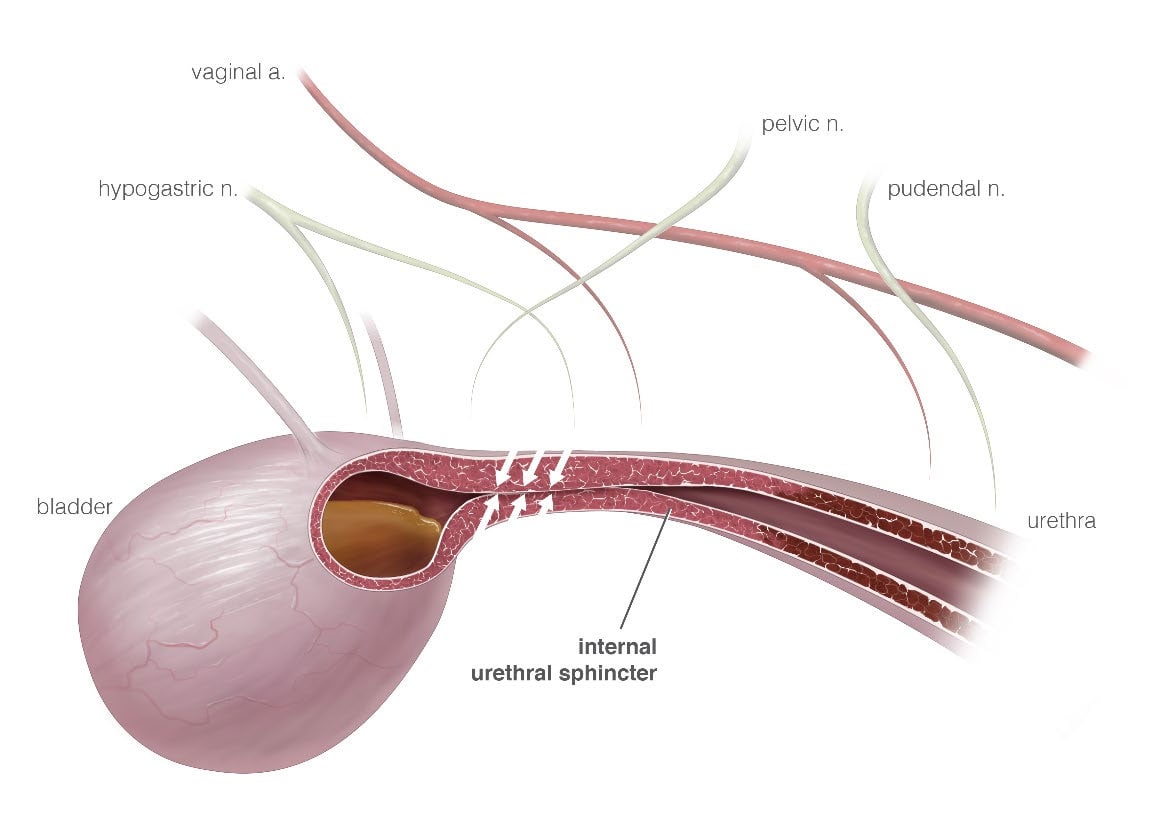
Although many risk factors for development of urinary incontinence have been identified in the dog, we are still unsure of the mechanism of its development. It is likely a multifactorial process that involves the pituitary-gonadal axis and tissue mechanics. Several things are important in the maintenance of a closed urethra (Figure 1). These include vascular tone (which can represent up to 30% of closure pressure), the strength of supporting structures in the pelvic region, and the positioning of the bladder. Some studies have implicated a rise in luteinizing hormone (LH) and gonadotrophin releasing hormone (GnRH) levels as well as increases in their receptors in female animals secondary to the decline in estrogen levels after neutering. These changes may have an impact on smooth muscle contractility in the lower urinary tract. In support of this theory, one study has shown that the administration of GnRH analogues to dogs with USMI can lead to improvement of continence.
Figure 1: Schematic of the smooth muscle internal urethral sphincter
Estrogen has trophic effects on the vasculature and tissue matrix of the lower urinary tract and its support structures in women. The decline in estrogen levels can cause a decrease in the vasculature of the urethra and its supporting tissues, which is an important part of maintaining a closed urethra. There is also a possibility that the collagen content may be altered in females with USMI, however, further studies are needed.
Another important factor in the maintenance of continence is the positioning of the bladder. In the normal animal intra-abdominal pressure transmits to the bladder and the proximal urethra. This equalizes the pressure between the bladder and its outflow tract, preventing leakage. In dogs with a caudally positioned bladder (“pelvic bladder”) the pressure increases that occur with movement, barking, and coughing transmit to the bladder and not the urethra, and thus create a pressure gradient from the bladder to the urethra, resulting in leakage. This may be more common in some breeds such as Greyhounds, Doberman Pinschers, and Weimeraner.
In women, urinary incontinence is often caused by detrusor hyperreflexia or “overactive bladder”. This condition occurs when the bladder spontaneously contracts without reaching full capacity resulting in the leakage of urine. This condition is treated with anti-muscarinic drugs such as oxybutynin and imiprimine. Some studies have suggested that this condition may occur in dogs with urinary incontinence, however, the definitive diagnosis relies on urodynamic testing. In lieu of this procedure, some practitioners will place patients on these medications if they fail to respond to alpha-agonist and estrogen therapy.
Treatment of Urethral Sphincter Mechanism Incompetence
In the majority of USMI cases, otherwise healthy patients are treated initially with either alpha-agonist medications such as phenylpropanolamine (Proin, PRN Pharmacal) or estrogen compounds like DES or estriol (Incurin, Merck Animal Health). Alpha-agonists increase the stimulation of the adrenergic receptors on the internal urethral sphincter while estrogens may up-regulate the expression of such receptors. There is anecdotal evidence that the two drugs in combination may be synergistic and benefit patients who do not respond to either drug alone. We recommend performing a baseline systolic blood pressure before starting phenylpropanolamine since hypertension is a potential side effect of alpha agonist therapy. The dog should also have its blood pressure monitored after 2-4 weeks on the medication. Other adverse effects of phenylpropanolamine include restlessness, aggression, decreased appetite, and insomnia. Side effects of estrogen therapy include mammary and vulvar swelling and attractiveness to male dogs. These side effects generally resolve when the medication is decreased or stopped.
Figure 2: Placement of bovine cross-linked collagen as a urethral bulking agent
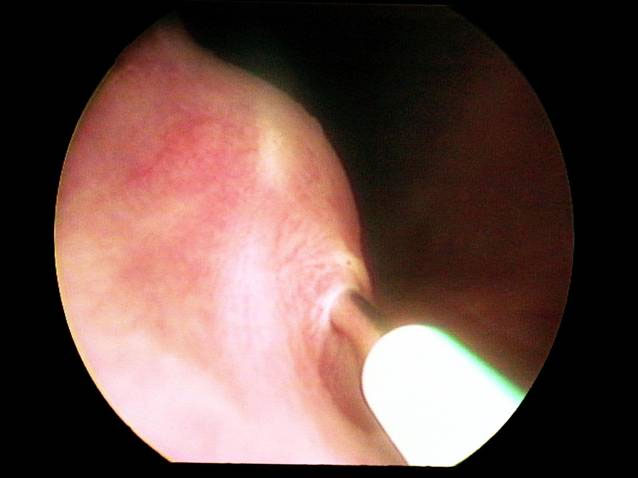
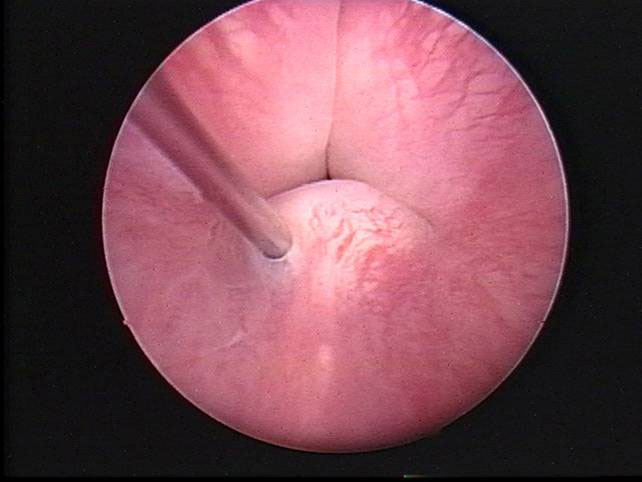
Surgical therapy of urinary incontinence has focused on increasing the transmission of intraabdominal pressure to the proximal urethra and improving the stability and pressure within the urethra. Colposuspension, which attaches the uterine remnant to the pelvic ligament and thus draws the bladder neck and proximal urethra further into the abdomen, has been found to have variable success and has a high failure rate due to breakdown of the attachment to the pelvic ligament.
Male dogs with urinary incontinence pose a more difficult challenge. Less than 50% of male dogs respond to medical therapy, and the most successful treatment is PPA. Testosterone cypionate has had some anecdotal use and may provide some improvement. Alternative treatment in males that fail medical therapy include surgical placement of an artificial urethral sphincter and urethral collagen injections, which may be performed antegrade through a cystotomy incision, or retrograde via perineal urethrotomy.
Functional Urethral Obstruction
The poor response of male dogs with urinary incontinence to traditional USMI therapy may be due misdiagnosis. It is likely that many of these dogs have overflow incontinence secondary to an inability to empty their bladder rather than a weak urethral sphincter. The etiology of functional obstruction or DUD is elusive, and may involve the reticulospinal tract. The net effect is incoordination between the reflexive relaxation of the urethral smooth and skeletal muscle when the bladder contracts. It appears that the obstruction can involve either the smooth or skeletal muscle of the urethra, or a combination.
The diagnosis is made by assessing urine stream and residual urine volume. Normal dogs should have less than 1-2 ml/kg of urine in their bladders after a normal void. Some dogs with DUD will have greater than 15 ml/kg. Other causes of obstruction must be ruled out such as strictures, uroliths, and extramural compressive lesions before a diagnosis of DUD can be made. This can be easily accomplished with contrast cystourethrography. This may also assist in guiding therapy, since the location of the most resistance usually sits just distal to an abnormally wide portion of the urethra on such a study.
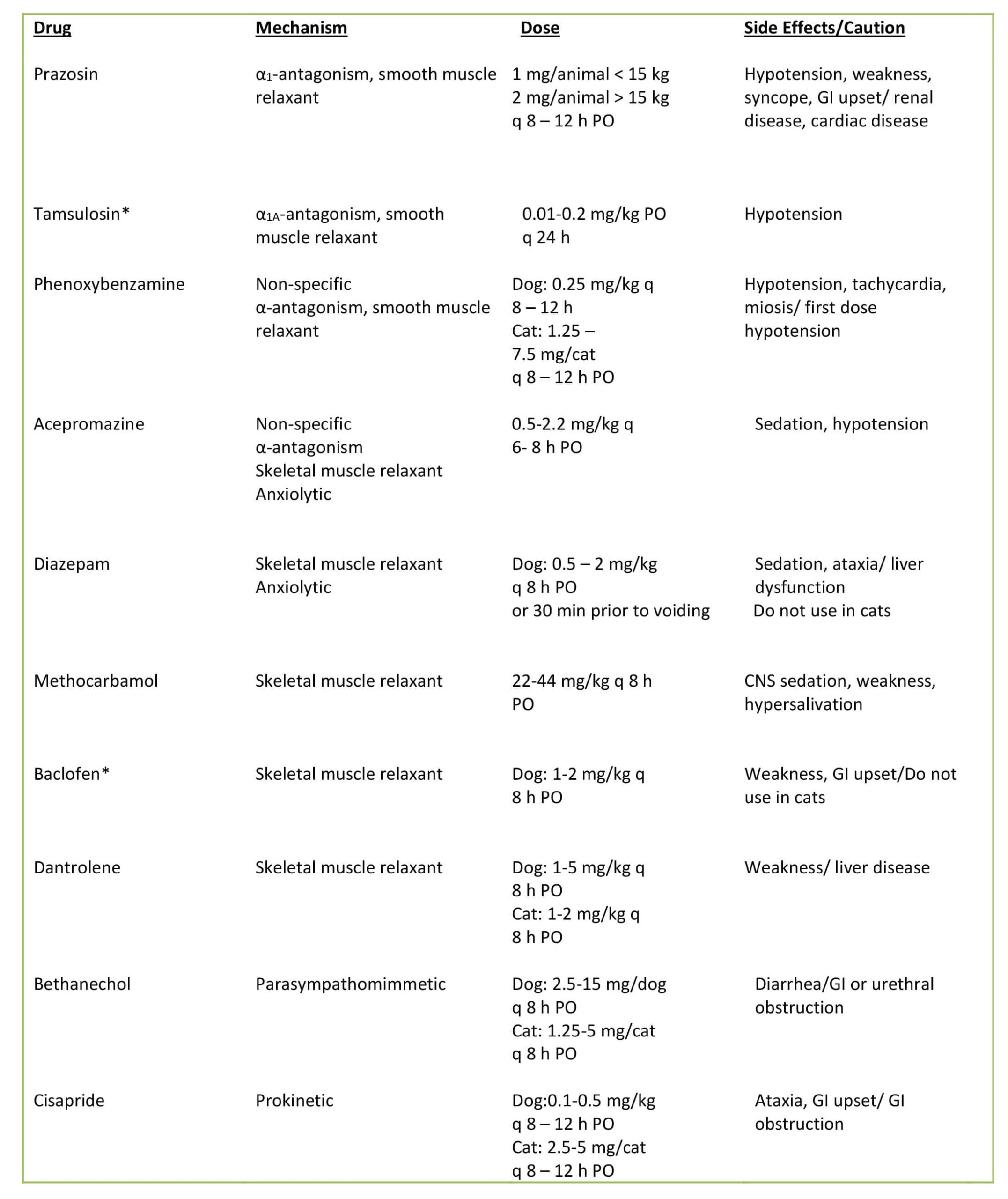
Medical treatment for DUD generally consists of muscle relaxation, and occasionally anxiolytic therapy. The prostatic urethra contains primarily smooth muscle and the penile urethra contains primarily skeletal muscle. The perineal urethra is a combination of the two types. It is often necessary to use both smooth and skeletal muscle relaxants in these patients to achieve the desired result. The most commonly used medications are listed in Table 1. Alpha receptor antagonists are a mainstay of smooth muscle relaxation, while the addition of low doses of diazepam just before urination can relax the skeletal muscles. Some dogs exhibit a worsening of clinical signs when stressed or anxious, and these patients may benefit from trazadone, fluoxetine, or other anxiolytic medication. Clients should be instructed on indications for and technique of urethral catheterization in their male dog. This can prevent costly emergency visits and provide temporary relief to the dog.
There is very little information as to the long-term outcomes in male dogs with DUD and the evidence for treatment efficacy is lacking. Some patients may require significant dose adjustment of medications in order to determine the optimal therapy. Dogs that do not respond to treatment may require urethral stenting, although this is considered a salvage procedure and may lead to significant adverse effects.
Table 1: Drugs frequently used to treat disorders of emptying
Conclusion
The mechanisms behind urinary incontinence in the dog are multilayered and poorly understood. Treatment must be tailored to focus on whether the problem involves an inability to hold urine during bladder filling, or to empty the bladder completely during active urination. Medical therapy is directed at the smooth muscle, and sometimes skeletal muscle of the urethra to either improve contraction or enhance relaxation. There are some surgical and cystoscopic interventions which may improve the outcome in these patients when medical therapy fails.